Injuries to the mouth, face and jaws
Brief description of the condition
Trauma to the head and neck can result in injuries to the teeth and/or the surrounding tissues and structures in the mouth, face and jaws. This takes various forms and can be broadly categorised as:
- dentoalveolar injuries, including broken, displaced or lost teeth and injuries to the supporting bone
- maxillofacial fractures and soft tissue injuries, including fractures of the mandible and maxilla and lacerations to the mucous membranes lining the oral cavity.
Non-accidental injury
In all cases of injury caused by trauma, health care providers need to have a high level of suspicion for non-accidental injury (NAI), particularly injuries in children and vulnerable adults and potential domestic abuse in adults. There is a need to differentiate between NAI and accidental injury, taking into account the behaviour of the patient and of anyone accompanying them, in addition to the history and presentation of the injury. Speaking to the patient without the accompanying person being present, if possible, can be helpful.
Follow local procedures for reporting concerns if NAI is suspected in a child or vulnerable adult, or there is suspected domestic abuse with children at home.42,43 For suspected domestic abuse, consider direction to resources for support (e.g. Scotland’s Domestic Abuse and Forced Marriage Helpline; National Domestic Abuse Helpline).
Key signs and symptoms
Dento-alveolar Injuries
- Pain
- Bleeding
- Fracture of tooth or loss of tooth structure
- Increased mobility of tooth or several teeth as a unit
- Tooth looks displaced or elongated
- Empty tooth socket
Maxillo-facial Fractures and Soft Tissue Injuries
- Pain exacerbated by movement
- Bleeding
- Swelling
- Teeth/dentures do not meet together in the way that they did before
- Tooth mobility
- Paraesthesia (tingling, prickling, pins and needles, or burning sensations)
- Other problems specific to bone fractures e.g. nose bleeds, diplopia (double vision), loss of visual acuity
Initial management
Determine if the patient is in need of emergency medical attention (e.g. bleeding is severe and will not stop within 15-30 minutes; there has been significant facial trauma; the patient has had a head injury or loss of consciousness; inhalation of tooth or tooth fragment; airway obstruction).
If in need of emergency medical attention, send the patient for emergency medical care at the nearest emergency department or if the patient is not safe to move, call 999. Be aware of the risk of cervical spine injury in deciding whether to move a patient.
If not in need of emergency medical attention:
- Clean the affected area by rinsing gently (e.g. with salt water or saline if available) and if foreign object(s) are present in the mouth, remove them.
- Apply pressure with damp gauze, clean handkerchief or a finger to stop any bleeding.
- Apply ice packs to soft tissue injury and swelling.
If a permanent (NOT primary¥) tooth has been knocked out (avulsed):
Advise immediate reimplantation of the tooth, if feasible, as follows:44
- handle the tooth by its crown (the white part), avoid touching the root
- if the tooth is dirty, rinse it gently in milk, saline or in the patient's saliva
- immediately reimplant the tooth in its original position in the jaw and then bite gently on a clean handkerchief or gauze to hold it in position
-
- if available, a mouthguard, bleaching tray or foil bandage can be used to hold the tooth in position and reduce the risk of periodontal ligament cells drying out
- advise the patient to seek emergency dental care*
If reimplantation is not feasible:
- immediately place the tooth in milk, saliva (e.g. after spitting into a container) or saline for transportation to the dentist
- alternatively transport the tooth in the mouth, keeping it between molars and the inside of the cheek (this may not be appropriate for children due to the risk of choking)
- avoid the tooth becoming dry
- advise the patient to seek emergency dental care*
Consider recommending analgesia (see Analgesia). Do not prescribe antibiotics.
The patient should be advised of the importance of reimplanting the tooth immediately where feasible, and that prolonged storage rather than reimplantation will decrease longevity of the tooth due to increased risk of resorption. A self-help video for patients demonstrating reimplantation of a tooth is available on the Dental Trauma UK website.
* An avulsed permanent tooth with no other complications is a dental emergency but not a medical emergency. During the out of hours period, hospital emergency departments may not be able to provide timely or appropriate dental care, particularly if OMFS services are not available. The patient/carer should be advised to immediately reimplant the tooth, if feasible, and if emergency dental clinics are closed, may be directed to the first available emergency dental clinic appointment.
If a primary¥ tooth has been knocked out (avulsed):
Do not reimplant.45 Seek non-urgent dental care, or urgent dental care if there other concerns, for example possible intrusion of tooth (i.e. the tooth cannot be located and may have been completely pushed back into the gum) or safeguarding concerns.
¥A guide to the age at which permanent teeth appear in the mouth is available at https://www.mouthhealthy.org/all-topics-a-z/eruption-charts. This may be of help when identifying whether a tooth is permanent or primary.
If a permanent tooth¥ (or teeth) has been moved out of its usual position, advise the patient to seek urgent dental care for assessment.
If a primary tooth¥ (or teeth) has been moved out of its usual position, advise the patient to seek urgent dental care. Advise the parent/carer to alter the child’s diet to include soft food.
Note that a mobile tooth is unlikely to be an aspiration risk after the point of trauma and is not considered a dental emergency.
¥A guide to the age at which permanent teeth appear in the mouth is available at https://www.mouthhealthy.org/all-topics-a-z/eruption-charts. This may be of help when identifying whether a tooth is permanent or primary.
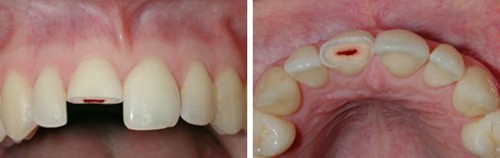
Fractured tooth involving the pulp
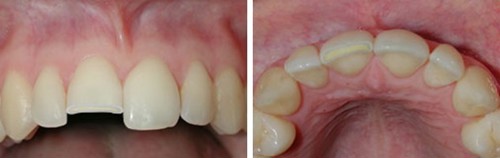
Fractured tooth involving enamel and dentine
Illustrations from the Dental Trauma Guide www.dentaltraumaguide.org
If a permanent tooth¥ fracture involves the dental pulp, advise the patient to seek urgent dental care and keep any broken pieces of tooth in milk, saline or water. If available, the patient could apply a temporary dressing/filling material.
If a permanent tooth¥ fracture involves only enamel and dentine, advise the patient to use desensitising toothpaste or a temporary dressing/filling material on the exposed dentine as a first aid measure, to keep any broken pieces of tooth in milk, saline or water and to seek urgent dental care for assessment.
Consider recommending analgesia (see Analgesia). Do not prescribe antibiotics.
¥A guide to the age at which permanent teeth appear in the mouth is available at https://www.mouthhealthy.org/all-topics-a-z/eruption-charts. This may be of help when identifying whether a tooth is permanent or primary.
If any facial fractures are suspected, send the patient to emergency medical care via NHS24/111. Dentoalveolar fractures, involving the supporting structures of the teeth only, should be managed via emergency dental care.46 Do not prescribe antibiotics at the initial assessment.
If the patient has oral lacerations that either:
- will not stop bleeding with sustained application of pressure
- involve the outside of the lip (greater than ~1 cm in length)
- cross the vermillion border on to the facial skin, or
- have resulted in the oral tissues being stripped from the underlying bone (degloving injury)
send the patient for emergency medical care via NHS24/111 ideally within 1 hour.
If the lacerations involve the attached gingival (hard gum) tissue and are greater than ~1 cm in length send the patient for emergency dental care.
Otherwise, soft tissue lacerations (less than 1 cm in length) with no other concomitant injuries do not usually require further operative care, unless failing to heal, but advise the patient to maintain good oral hygiene and to use salt water mouthwash.
Subsequent care
Subsequent care depends on the diagnosed condition and whether any tooth involved is primary or permanent.
Dento-alveolar injuries
Consider:
- Radiographic examination for complete diagnosis.
- Addressing permanent tooth fractures or loss of permanent tooth structure by restoring the tooth or re-bonding the fractured part of the tooth if available.
- Pulp capping, partial pulpotomy or, particularly for a primary tooth, extraction.
- Repositioning, splinting and subsequent root canal treatment for excessively mobile, displaced or reimplanted avulsed teeth, taking into consideration the maturity of the tooth and other relevant factors.44,46
-
- Root canal treatment should be carried out within 2 weeks of reimplantation of an avulsed tooth with a closed apex, or an avulsed tooth with an open apex which has had extra-oral dry time of more than 60 minutes.44
- Instructing the patient to adhere to a soft food diet for 7 days or for the duration of splinting.
Advise the patient to maintain good oral hygiene.
The International Association of Dental Traumatology guidelines for the management of traumatic dental injuries provide detailed advice on the management of avulsed teeth and a wide range of injuries and conditions that result from trauma.
Maxillo-facial fractures and soft tissue injuries
These conditions require specialist care and are normally managed by oral and maxillofacial surgery teams.